|
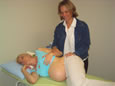
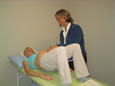
Common conditions and treatment options
Bladder and bowel problems: . Incontinence - 25% of adults have experienced leaking at some time - 34-40% of individuals over 65 have leaking problems - >50% of nursing home residents are incontinent Incontinence should NOT be accepted as normal after childbirth or menopause. Medical treatment models suggest that Pelvic Floor Exercise and habit changes can improve incontinence in 80% of cases (male and female). Pelvic floor strengthening with computerized biofeedback providing visual and auditory feedback, electrical stimulation, bladder retraining and behavioral modifications are conservative and proven treatments for incontinence. Physiotherapists need to be specialized in pelvic floor rehabilitation and have experience in this field to provide these services. We work closely with gynaecologists, urogynaecologists, urologists and family practitioners to find the best solution to reduce and eliminate symptoms. . Overactive bladder This is urgency/frequency with more than 9 visits to the toilet in 24 hours with or without leaking. Pelvic floor muscle weakness can be a cause and responds well to computerized biofeedback training, electrical stimulation and bladder retraining. Myofascial spasms of the pelvic, hip, or lower back muscles can also contribute to an abnormal urge sensation. We therefore do a detailed musculoskeletal evaluation to determine contributing factors. Treatment may include biofeedback, bladder retraining, electrical stimulation, myofascial release, stretching and specific strengthening exercises. . Chronic constipation/evacuation disorder People who are constipated often strain to pass stool thus continually overstretching the pelvic floor. A more relaxed evacuation technique can be taught to help prevent continued overstretching. Additionally diet, fluid intake and medication can be discussed in order to establish a more routine bowel habit. Pre- and Post- Operative Care Abdominal surgeries, including hysterectomy, removal of ovarian cysts, or hernia repair, may disrupt the abdominal muscles. Hospital stays following surgery have shortened. After surgery, you may be afraid to move. Abdominal muscles disturbed during surgery may be weakened, and may continue to weaken as you lie in bed. Weak muscles make moving more difficult and lead to poor posture. Now, more than ever, you should take an active part in recovering from your abdominal surgery. Also, you can help yourself recover with exercises or other self care activities after you go home. A physiotherapist can evaluate your problem and help manage the debilitating effects of abdominal surgery. Your physiotherapist may teach you circulatory exercises, correct coughing and moving techniques to reduce stress on the wound, exercises and self-help techniques to encourage bowel activity and reduce post-surgical pain from gas, relaxation training, scar tissue mobilization, an individualized home exercise programme for your back, pelvic and abdominal muscles and ergonomic training to reduce pressure on the scar with lifting and everyday activities. Pelvic Pain Conditions Conditions such as vulvodynia, vaginismus, levator ani syndrome, pelvic floor tension myalgia, interstitial cystitis, dyspareunia (painful intercourse), sacro-iliac (SI) joint dysfunction, coccydynia (tailbone pain) for example, often have musculoskeletal components that can be successfully treated by a skilled and specialized physiotherapist. Many of these conditions are multi-dimensional and in many cases we will work with a multi-disciplinary team consisting of any or all of the following: family physician, gynecologist, urogynecologist, urologist and psychologist. After a thorough examination, treatment may include Travell trigger point release and stretches, Maitland/ McKenzie / Mulligan specific joint mobilizations, biofeedback, dilators, specific strengthening / stretching exercises and self-treatment techniques. Ante- and Postnatal Care The childbearing year brings dramatic changes to the body. Physiotherapy can assist you in managing these musculoskeletal changes. Conditions we often see during pregnancy are SI joint dysfunctions, sciatica, carpal tunnel syndrome, plantar fasciitis, lower back, neck or thoracic pain and headaches. Postpartum we treat weak pelvic floor muscles with or without incontinence, rehabilitation of lower abdominals or "core" muscles which assist in preventing lower back / pelvic pain, painful episiotomy scars and other common orthopaedic dysfunctions. Interestingly, in some countries like France and Sweden, women routinely get 2-4 sessions with a physiotherapist 6-8 weeks postpartum for pelvic floor strengthening, lower back stabilization training and postural and kinetic handling training. All new moms are advised to have a postnatal physiotherapy check at 6 weeks, to assess pelvic floor and abdominal muscles, irrespective of whether you had a Caesarian section or natural childbirth. Osteoporosis Women at risk for, or with, osteoporosis need to increase weight-bearing exercise, improve balance and decrease postural strain. Your physiotherapist will do a thorough evaluation and develop a customized exercise programme to address these issues. Behavioral Modifications A lot of our toilet behavior is formed through habit. No-one teaches us how to empty the bladder, or evacuate the bowels. Often we learn bad habits along the way. Common examples: . Going to the toilet "just in case" can decrease the bladder volume and increase urinary frequency, worsening the problem. . Straining when evacuating the bowels decreases the body's ability to "expel" fecal matter, resulting in the need to strain, worsening the situation. 1)Bladder Training (Drill) You may be suffering from urgency, which is the urgent need to get to the toilet before you have an accident and sometimes you may not make it on time. The bladder can learn bad habits, often over a period of years. Eventually, the bladder starts to dictate when it should be emptied rather than allowing for you to decide when it's convenient for you. It is possible to train the bladder so that you can have more control over it resulting in less frequent trips to the bathroom. It may be useful to keep a bladder diary for a few days to record how often you urinate and thus you can set yourself goals to increase the time between visits. If you encourage the bladder to hold on, it will get used to holding more urine before telling you it urgently needs to get to the bathroom. Therefore you will not experience as many urges and subsequently you will go to the bathroom less often. It is best to start your training when you are at home as accidents can happen in the initial stages, when you are trying to hold for longer. It is possible to calm down an urge by taking control of the situation. To regain control of your bladder it is necessary to "train" it: . Don't empty the bladder "just in case". If you need to go more than every 2 hours try to wait a little longer, even a few minutes will help to stretch the bladder and encourage it to hold better. . When you get an urge to go, don't PANIC, keep as calm as possible and try to hold a gentle pelvic floor contraction (not as hard as possible, but hard enough to prevent leaking) for about 20 seconds, or as long as able. The desperate urge should pass! This should allow you to last another minute or two, or to get to the toilet without leaking. Sometimes the urge may pass completely and you may go half an hour before you get it again! . If you are able to sit down, cross your legs and point your toes. If you are unable to sit down you try standing on your tip toes, crossing your legs and rubbing the backs of your thighs. These postures set off reflexes that calm the activity of the bladder. . Do not restrict your fluid intake. The less fluid, the stronger the urge and the more irritable the bladder becomes. Try to drink at least 1.2 litres or 4-6 glasses. Water is the best! . Some bladders are more sensitive to caffeine. This is found in coffee, tea, and believe it or not, CHOCOLATE! Reducing your intake of caffeine, ALCOHOL, acidic foods (vinegar), and spicy foods may decrease your urinary frequency. . If you wake up at night to empty your bladder, don't drink within 2 hours of going to bed. PERSEVERE! Bladder training takes at least 6 weeks before it has a noticeable effect. 2) Evacuation technique (Getting things moving) There is a position that encourages the bowels to move freely and the pelvic floor to relax. This promotes bowel emptying without straining. Straining can damage the muscles of the pelvic floor by stretching them. . The knees should be higher than the hips. To achieve this, the feet should be supported on a box, or pile of magazines and raised about 10-15 cm's. . Lean forward, keeping the back straight and let the abdomen relax. . Rest the elbows on your knees. . Relax the pelvic floor muscles. . "Strain" by allowing the abdomen to swell forwards and the waist to swell sideways. . DO NOT hold the breath and push. . Open the mouth and whisper 'Pah-ha-ha' on the breath out. . Keep breathing until the urge to push comes. Push gently. . If no success: Relax, lean back and wait a few seconds. Resume the above position and try again. Pelvic Floor Exercises: 1) Sit/lie comfortably with your thighs and buttocks relaxed 2) Tighten the ring of muscle around the back passage, vagina and front passage (as if trying to stop passing wind and urine at the same time). You should feel a lifting up and inwards as you tighten. It is very difficult not to use other muscles as well. Do not squeeze your buttocks or thighs. It is essential that you BREATHE throughout the exercises. Try to tighten the muscles at the end of a breath out. If you are doing it correctly, no one should notice you are doing the exercises just by looking at you! 3) Everybody differs in the length of time they can squeeze, and how many repetitions they can do before fatigue. When you release, you should have a definite feeling of letting go. There are 3 main types of Pelvic Floor contractions: a) Strong slow squeezes (70-80% effort) Tighten your pelvic floor, and hold the contraction. Focus on letting go when you relax. Do ____ repetitions for ____seconds. Do this ____ times/day. As your muscles get stronger, you will be able to hold for longer periods of time. Start with 5 seconds and progress slowly until you can do 10 second squeezes for 10 repetitions. b) Fast squeezes (90-100 % effort) It is important for these muscles to learn to contract quickly, so that they can activate quickly when you cough or sneeze. Tighten the pelvic floor muscles and let go immediately, without holding. Do ____ fast contractions ____ times per day. c) Gentle long holds (20-50% effort) It is beneficial to train the pelvic floor muscles to hold for longer periods of time (not as hard as you can, but enough to be "aware of" a contraction). Try to squeeze at less than 20-50% of your maximum effort for 20 seconds and upwards. If you get good at this, try to do it while doing other things e.g. washing the dishes, preparing dinner, talking on the phone, waiting in a queue, etc. |